Introduction to Ticlopidine and Its Use in Medicine
In the world of medicine, Ticlopidine is a name that many of us may not be familiar with, but it plays an essential role in the treatment of certain conditions. As a blogger, I've spent time researching this drug and its uses. Ticlopidine is an antiplatelet drug, often used to prevent stroke in patients who cannot tolerate aspirin or in those for whom aspirin is not effective. It works by preventing platelets in your blood from sticking together to form harmful clots.
Exploring the Concept of Drug Resistance
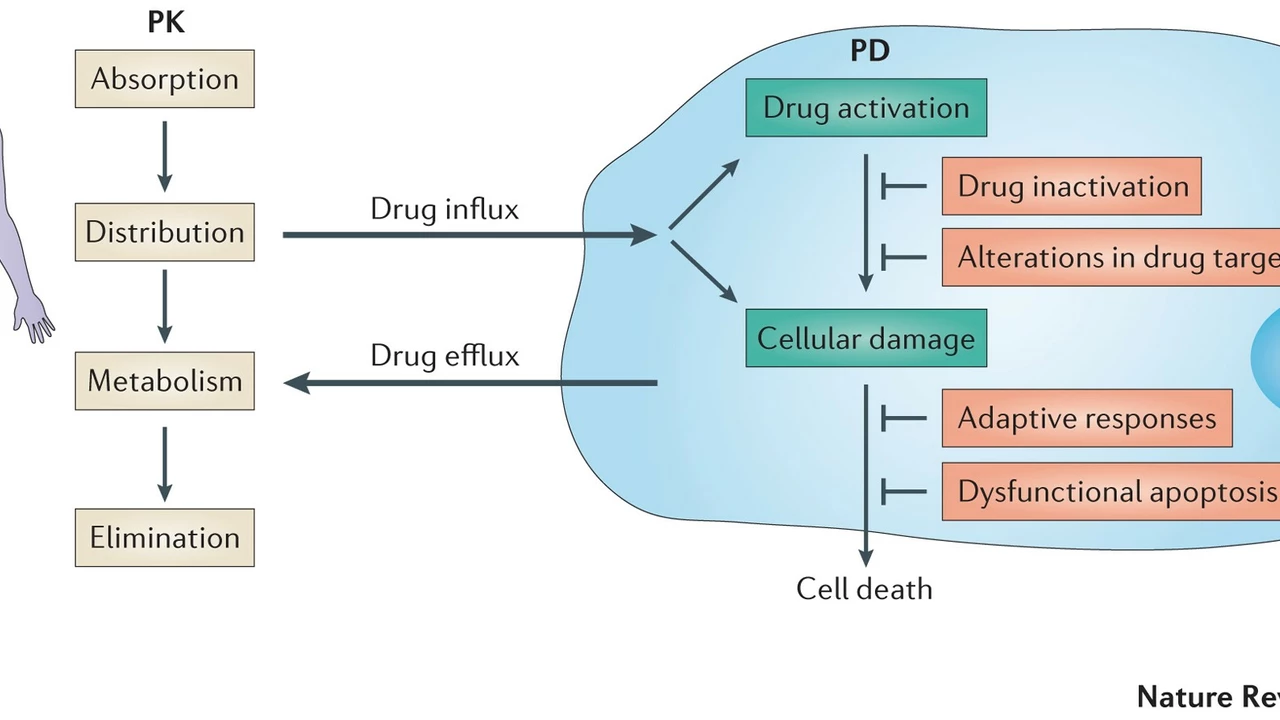
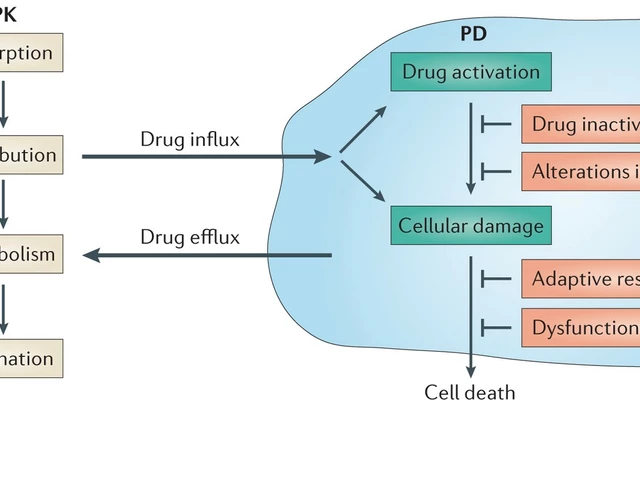
Drug resistance is a phenomenon that occurs when a drug that was once effective in treating a condition becomes less efficient or completely ineffective. The reasons behind this can be complex, ranging from genetic mutations in the target of the drug to changes in the body's absorption, distribution, metabolism, or elimination of the drug. In the case of Ticlopidine, resistance can occur and lead to treatment failure, which is a significant concern for physicians and patients alike.
The Mechanism of Ticlopidine Resistance
Understanding the mechanism of Ticlopidine resistance is crucial to addressing the problem. Researchers believe that the resistance to Ticlopidine primarily arises from the genetic variability of the patient. Genetic factors can affect how the body metabolizes the drug, and this can lead to resistance. Furthermore, some patients might have a higher number of platelets, which might reduce the drug's effectiveness.
Signs and Symptoms of Ticlopidine Resistance
Identifying Ticlopidine resistance in patients is a challenging task. Commonly, the resistance is identified when patients continue to experience symptoms or have recurrent strokes despite being on Ticlopidine therapy. However, it's vital to remember that every patient is unique, and the signs of resistance can vary from one individual to another.
Diagnosing Ticlopidine Resistance
Diagnosing Ticlopidine resistance involves a series of steps. Doctors will first assess the patient's symptoms and medical history. Next, they may order blood tests to check for the presence and activity of the drug in the bloodstream. In some cases, genetic testing may also be done to determine if the patient has certain genetic traits that may contribute to resistance.
Managing Ticlopidine Resistance
Managing Ticlopidine resistance is a complex process and often involves a multidisciplinary approach. The first step is usually to adjust the dosage or switch to a different medication. In some cases, combining Ticlopidine with other drugs may help to overcome resistance. It's essential to work closely with healthcare professionals in these situations to ensure the best possible outcome.
Preventing Ticlopidine Resistance
Preventing Ticlopidine resistance is a challenging task, but it's not impossible. It involves a combination of strategies such as regular monitoring of drug levels in the blood, genetic testing, and patient education. By understanding the risk factors for resistance and taking steps to mitigate them, we can optimize the treatment outcomes for patients on Ticlopidine therapy.
Implications of Ticlopidine Resistance
The implications of Ticlopidine resistance are far-reaching. For patients, it may mean a higher risk of stroke and other related complications. For healthcare systems, it could lead to increased healthcare costs due to the need for more intensive treatment and monitoring. Therefore, understanding and addressing Ticlopidine resistance is of utmost importance.
The Future of Ticlopidine Therapy
Looking towards the future, researchers are tirelessly working to find ways to overcome Ticlopidine resistance. The development of new drugs and the refinement of existing ones are a significant part of this effort. Additionally, personalized medicine, which involves tailoring treatment to an individual's unique genetic profile, holds great promise in this field.
Conclusion: The Importance of Understanding Ticlopidine Resistance
In conclusion, understanding Ticlopidine resistance is vital for both healthcare professionals and patients. It's a complex issue with many factors at play, but with continued research and advancement in medical technology, we can hope for better strategies to manage and overcome this challenge. As we continue to learn more about this topic, we will be better equipped to provide effective treatment and improve the outcomes for patients.

james landon
July 7, 2023 AT 01:05Jenn Clark
July 8, 2023 AT 00:36L Walker
July 8, 2023 AT 19:55giri pranata
July 9, 2023 AT 16:44Kent Anhari
July 10, 2023 AT 00:44Charlos Thompson
July 10, 2023 AT 20:26Peter Feldges
July 11, 2023 AT 17:08Richard Kang
July 12, 2023 AT 11:46Rohit Nair
July 12, 2023 AT 23:32Wendy Stanford
July 13, 2023 AT 05:47